Ulcerative Colitis - children - discharge
Definition
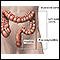
Your child was in the hospital because they have ulcerative colitis (UC). This is swelling of the inner lining of the colon and rectum (large intestine). It damages the lining, causing it to bleed or ooze mucus or pus.
|
Alternative Names
UC - children; Inflammatory bowel disease in children - UC; Ulcerative proctitis - children; Colitis in children - UC
When You're in the Hospital
Your child probably received fluids through an intravenous (IV) tube in their vein. They may have received:
- A blood transfusion
- Nutrition through a feeding tube or IV
- Medicines to help stop diarrhea
Your child may have been given medicines to reduce swelling, prevent or fight infection, or help their immune system.
Your child may have had surgery, such as:
- Removal of the colon (colectomy)
- Removal of the colon and most of the rectum
- Placement of an ileostomy
- Removal of a part of the colon
What to Expect at Home
Your child will likely have long breaks between flare-ups of ulcerative colitis.
Your Child's Diet
When your child first goes home, they may need to drink only liquids or eat different foods from what they normally eat. Follow the instructions given by your child's health care provider. Ask the provider when you can start your child's regular diet.
You should give your child:
- A well-balanced, healthy diet. It is important that your child get enough calories, protein, and nutrients from a variety of food groups.
- A diet low in saturated fats and sugar.
- Small, frequent meals and plenty of liquids.
Certain foods and drinks can make your child's symptoms worse. These foods may cause problems for them all the time or only during a flare-up.
Try to avoid the following foods that can make your child's symptoms worse:
- Too much fiber may make symptoms worse. Try baking or stewing fruits and vegetables if eating them raw bothers your child.
- Avoid giving foods that are known to cause gas, such as beans, spicy food, cabbage, broccoli, cauliflower, raw fruit juices, and fruits, especially citrus fruits.
- Avoid or limit caffeine, as it may make diarrhea worse. Foods such as some sodas, energy drinks, tea, and chocolate can contain caffeine.
Ask the provider about extra vitamins and minerals your child may need, including:
- Iron supplements (if they are anemic)
- Nutrition supplements
- Calcium and vitamin D supplements to help keep their bones strong
Talk with a dietitian to make sure your child is getting proper nutrition. Be sure to do this if your child has lost weight or their diet becomes very limited.
Managing Stress
Your child may feel worried about having a bowel accident, embarrassed, or even feel sad or depressed. They may find it difficult to participate in activities at school. You can support your child and help them understand how to live with the disease.
These tips can help you manage your child's ulcerative colitis:
- Try to talk openly with your child. Answer their questions about their condition.
- Help your child be active. Talk with your child's provider about exercises and activities that they can do.
- Simple things such as doing yoga or tai chi, listening to music, reading, meditation, or soaking in a warm bath can relax your child and help reduce stress.
- Have your child see a counselor who can help them gain self-confidence.
- Be alert if your child is losing interest in school, friends, and activities. If you think your child may be depressed, talk with a mental health counselor.
You may want to join a support group to help you and your child manage the disease. Crohn's & Colitis Foundation of America (CCFA) is one of such groups. CCFA offers a list of resources, a database of doctors who specialize in treating ulcerative colitis, information about local support groups, and a website for teens - www.crohnscolitisfoundation.org/patientsandcaregivers/justlikeme.
Medicines
Your child's provider may give them some medicines to help relieve their symptoms. Based on how severe their ulcerative colitis is and how they respond to treatment, they may need to take one or more of these medicines:
- Anti-diarrhea medicines can help when they have bad diarrhea. You can buy loperamide (Imodium) without a prescription. Always talk to their provider before using these medicines as sometimes they are not recommended to use in ulcerative colitis.
- Fiber supplements may help their symptoms. You can buy psyllium powder (Metamucil) or methylcellulose (Citrucel) without a prescription.
- Always talk to your child's provider before using any laxative medicines.
- You may use acetaminophen for mild pain. Medicines such as aspirin, ibuprofen, or naproxen may make their symptoms worse. Young children should not be given aspirin. Talk to their provider before taking these medicines. Your child may also need a prescription for stronger pain medicines.
There are many types of medicines available to prevent or treat attacks of your child's ulcerative colitis. The goals of treatment are to put the disease into remission, keep the disease inactive, and allow your child to feel well again.
Follow-up
Your child's ongoing care will be based on their needs. The provider will tell you when your child should return for an exam of the inside of their rectum and colon through a flexible tube (sigmoidoscopy or colonoscopy). Blood and stool tests may be done when your child is diagnosed, and then again at certain intervals to follow the disease.
When to Call the Doctor
Contact the provider if your child has:
- Cramps or pain in the lower stomach area that do not go away
- Bloody diarrhea, often with mucus or pus
- Diarrhea that cannot be controlled with diet changes and drugs
- Rectal bleeding, drainage, or sores
- New rectal pain
- Fever that lasts more than 2 or 3 days or a fever higher than 100.4°F (38°C) without an explanation
- Nausea and vomiting that lasts more than a day
- Skin sores or lesions that do not heal
- Joint pain that keeps your child from doing everyday activities
- A feeling of having little warning before needing to have a bowel movement
- A need to wake up from sleeping to have a bowel movement
- Failure to gain weight, a concern for your growing infant or child
- Side effects from any medicines prescribed for your child's condition
References
Bitton S, Markowitz JF. Ulcerative colitis in children and adolescents. In: Wyllie R, Hyams JS, Kay M, eds. Pediatric Gastrointestinal and Liver Disease. 6th ed. Philadelphia, PA: Elsevier; 2021:chap 43.
Stein RE, Anupindi SA, Baldassano RN. Inflammatory bowel disease. In: Kliegman RM, St. Geme JW, Blum NJ, eds, et al. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 382.
Velazco CS, McMahon L, Ostlie DJ. Inflammatory bowel disease. In: Holcomb GW, Murphy JP, St. Peter SD, eds. Holcomb and Ashcraft's Pediatric Surgery. 7th ed. Philadelphia, PA: Elsevier; 2020:chap 41.
Reviewed By: Jenifer K. Lehrer, MD, Gastroenterologist, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.